This month we are recognizing National Suicide Awareness and Prevention Month. Communities across the country are coming together to discuss ways to help prevent this public health crisis that takes the life of one person every 15 minutes (42,000 annually). Suicide is now the 10th leading cause for death for all ages and impacts individuals, families, and communities.
Although no one solution solves a complex problem like suicide, communities are making progress by collaborating with primary, behavioral health, and community service organizations to coordinate care for at-risk individuals. Two great examples are the state of New York and the state of Minnesota.
New York
The Substance Abuse and Mental Health Services Administration (SAMSHA) discovered that up to 45% of individuals who die by suicide have visited their primary care physician within a month of their death. With this alarming statistic in mind, SAMSHA provided the National Strategy for Suicide Prevention (NSSP) grant to New York to integrate suicide prevention into primary healthcare settings. With these funds the New York State Office of Mental Health developed their coordinated suicide prevention plan entitled, “1,700 Too Many.”
1,700 Too Many introduces a three-tiered strategy for success: community coordinated, data informed, and integrated suicide prevention into health and behavioral health settings. By incorporating these three concepts primary and behavioral health providers are encouraged to work together to coordinate an individual’s care, provide critical community supports and use data to continuously improve New York’s suicide prevention efforts.
Here is an overview of the New York State Suicide Prevention Strategy: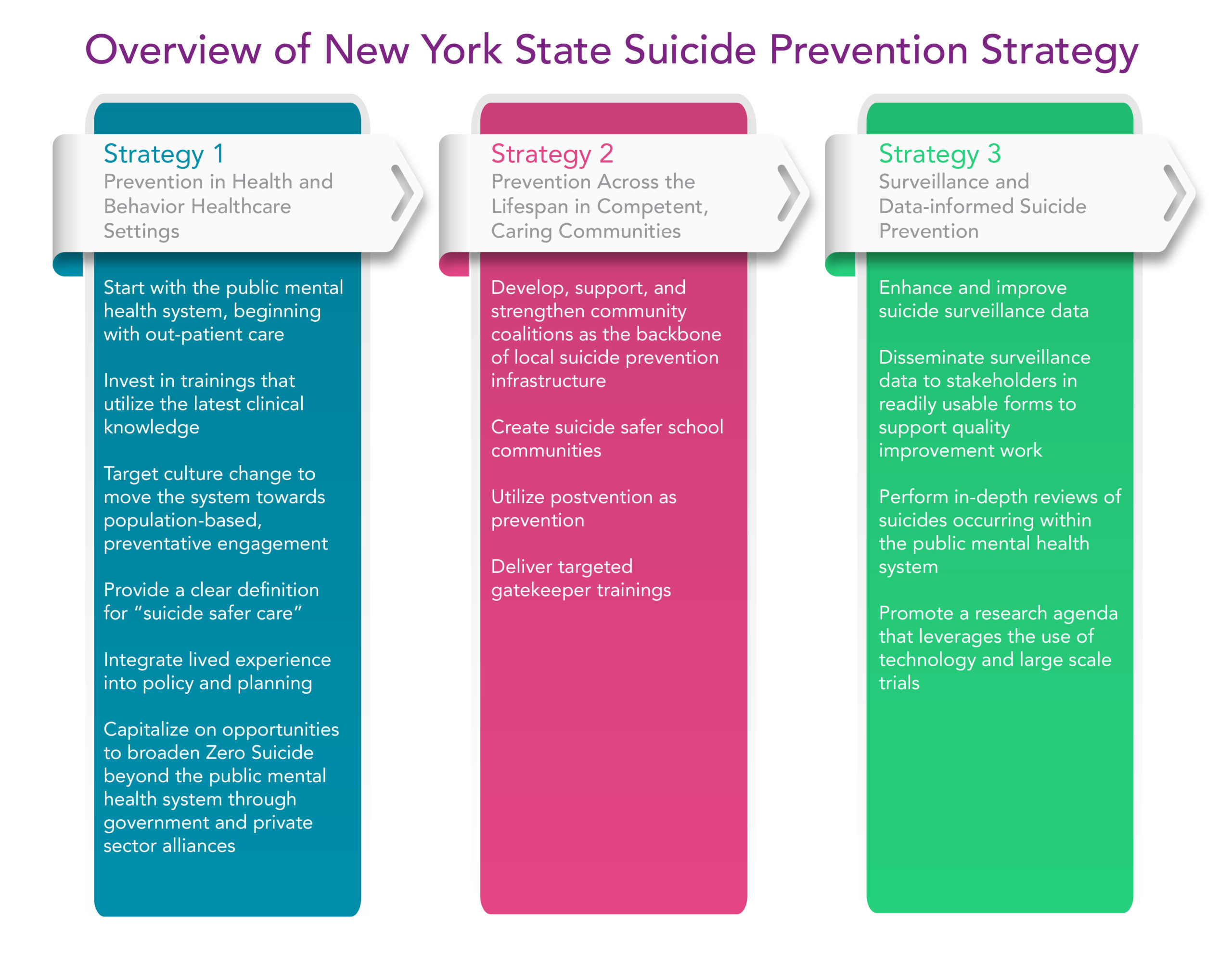
Minnesota
The state of Minnesota is another innovative leader in suicide prevention with its behavioral health home services (BHH) for Medicaid enrollees. Individuals who suffer from serious mental illness are at greater risk for suicide. They experience known barriers to healthcare access, high co-occurrence of chronic health conditions, and early mortality. Minnesota introduced the BHH model in July 2016 to provide whole-person care for these individuals, including primary care, mental health, substance use treatment, long-term services and supports, and social services through one multi-disciplinary team. According to the Minnesota Department of Human Services, BHH provides six core services:
- Comprehensive Case Management
- Care Coordination
- Health and Wellness Promotion
- Comprehensive Transition Care
- Individual and Family Supports
- Referral to Community Supports
The behavioral health home model is a win-win for both health providers and individuals struggling with mental illness as it improves the overall wellbeing of individuals and reduces care costs for providers.
Suicide is a serious concern. It is impossible to highlight everyone seeking innovative ways to care for individuals at risk. We here at Eccovia Solutions would like to salute everyone involved in supporting and encouraging these individuals to take a different path. It definitely takes the whole village.
Blog Resources
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4143796/
http://www.integration.samhsa.gov/about-us/esolutions-newsletter/suicide-prevention-in-primary-care
http://omh.ny.gov/omhweb/resources/publications/suicde-prevention-plan.pdf



