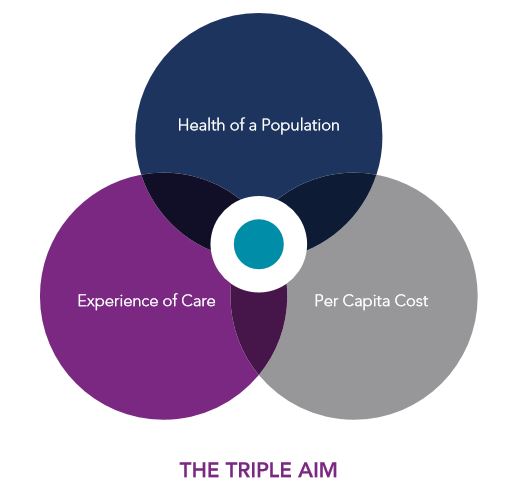
 Medicaid accountable care organizations (ACOs) are revolutionizing healthcare delivery for vulnerable populations. The goal of ACOs is to achieve the “Triple Aim” of healthcare: enhancing the patient experience of care, improving the health of the population, and reducing the per capita cost of care. ACOs are designed to connect providers’ reimbursement to the health outcomes of the population they serve (value-based healthcare) rather than basing reimbursement solely on the amount of services they provide (fee-for-service).
Medicaid accountable care organizations (ACOs) are revolutionizing healthcare delivery for vulnerable populations. The goal of ACOs is to achieve the “Triple Aim” of healthcare: enhancing the patient experience of care, improving the health of the population, and reducing the per capita cost of care. ACOs are designed to connect providers’ reimbursement to the health outcomes of the population they serve (value-based healthcare) rather than basing reimbursement solely on the amount of services they provide (fee-for-service).
The Center for Health Care Strategies identifies three key components of a community-based ACO: payment model, quality measurement approach, and data analysis strategies.
Payment Model
To establish a financial incentive for providers to deliver value instead of volume, states typically use one of the following models:
- Shared Savings Arrangement – Providers participating in an ACO have the opportunity to share in savings if their attributed population uses a less costly set of health care resources than a predetermined baseline (the “upside”). In some cases, providers transition over time to share the risk of providing more costly services (the “downside”), whereby they would pay the state back a percentage of costs if they exceed baseline numbers.
- Global Budget Model – ACOs receive a capitated per-patient payment to provide services and also accept full financial risk for the health of their patient population.
To determine how patient costs are measured under either model, states define the type of services offered under ACOs and calculate the predicted total cost of care of these services, either on a per-patient or population-wide basis. (Note: Some Medicaid ACO models include behavioral health, long-term services and supports, pharmaceuticals, and even social services in addition to physical health services.)
Quality Measurement Approach
In order to maintain the health of the population they serve, ACOs must carefully define a set of quality metrics that reflect the unique needs of their Medicaid population. Provider payments are tied to these quality metrics and providers typically will not receive a portion of shared savings if they exceed or do not meet quality benchmarks.
States are using a variety of quality matrix to access ACO outcomes, processes, and patient experience, including:
- ACO’s prior performance
- Statewide averages of other healthcare providers’ performance
- Performance of other ACOs
- Performance of other payer programs, such as the Medicare Shared Savings Program
Data Analysis Strategies
Medicaid ACO’s require substantial data to track patient utilization data and costs. Timely and accurate collection and analysis are essential to operation. This data can also be mined to identify opportunities to improve care management efforts. In order to ensure that correct data is available for analysis, ACOs must establish and maintain their own data infrastructure.
State Examples
Many states have begun to implement Medicaid ACOs with the goal of keeping patients healthy and costs manageable. Here are highlights of ACO programs in Colorado, Minnesota, Oregon, and Vermont.
Colorado
Colorado’s Accountable Care Collaborative (ACC) is made up of seven Regional Care Collaborative Organizations (RCCO) that coordinate healthcare across providers serving Medicaid enrollees. Colorado reported a statewide net savings of $29 to $33 million during Fiscal Year 2014, its third year of operation.
Minnesota
Minnesota’s provider-led Integrated Health Partnerships (IHPs) program started with six providers in 2013 and 10 more have joined since then. Minnesota requires IHPs to report on 32 quality metrics. By regulation, the participating providers must send the state the data necessary to calculate quality performance. The IHPs are then eligible to receive a portion of shared savings. Minnesota reported a savings of $76.3 million over the first two years of their program.
Oregon
Oregon’s Coordinated Care Organizations (CCOs) were established by the Oregon Health Authority to help the state reduce health care cost increases. Oregon’s CCOs have a global budget for all services provided for enrollees which grows at a fixed rate. Three percent of monthly payments to CCOs are held back by the Oregon Health Authority and then distributed as an incentive payment based on performance at the end of each year. Since 2011, ER visits decreased by 22 percent and hospital admissions for short-term complications from diabetes and chronic pulmonary disease decreased by 26.9 percent and 60 percent.
Vermont
In 2014 Vermont launched the Vermont Medicaid Shared Savings Program. In addition to primary care services, each Medicaid ACO is required to include community support services such as behavioral health, long-term services and supports, and pharmacy benefits. Vermont’s Medicaid ACOs use a dual-track payment structure. In Track 1, the ACO has an opportunity for shared savings and is not exposed to any downside risk. In Track 2, the ACO is exposed to downside risk with an opportunity for a greater percentage of shared savings than in Track 1. ACOs are able to select the track in which they will participate. Over the first year of their program, Vermont reported a savings of $14.6 million.
Accountable Care Organizations are revolutionizing healthcare delivery and care coordination for Medicaid beneficiaries across the country. Eccovia Solutions provides a powerful case management system that is specifically designed for the collaborative, highly integrated Medicaid Accountable Care Organization model. Our ClientTrack Case Management platform enables ACOs to incorporate the social determinants of health into healthcare decisions, link primary care and community services, and coordinate a seamless journey for clients.
To learn more
http://www.chcs.org/media/Medicaid-Accountable-Care-Organization-Programs-State-Profiles.pdf
http://www.chcs.org/media/ACO-LC-BH-Integration-Paper-0709141.pdf



